Acupuncture treatment at The House, Middlesbrough
Pain is something every human experiences. But when does it stop being a temporary warning signal and start becoming something more persistent?
Clinically, pain is generally considered chronic when it lasts longer than three months: beyond the window in which most tissues heal. At that point, the experience of pain is no longer about active injury. It's often about how the nervous system has learned to process signals, and that calls for a different kind of support.
In the clinic, I regularly meet people who say: "I thought this would have settled by now." They've had the scans. The GP has told them nothing is structurally wrong. And still, every morning, the pain is there.
If that sounds familiar, you're not alone. Understanding what's happening is often the first step toward feeling less stuck.
Key Takeaways
- Pain lasting longer than three months is generally considered chronic, but the timeline matters less than understanding what's maintaining it now.
- Chronic pain isn't a sign of weakness or imagination. It often reflects real, measurable changes in how the nervous system processes signals.
- Central sensitisation, where the brain and spinal cord stay on high alert, is a recognised mechanism behind many chronic pain conditions, including fibromyalgia and persistent back pain.
- Stress, emotional load, and previous injury all influence whether pain persists. The mind-body connection in chronic pain is physical, not imagined.
- NICE recommends acupuncture as a first-line treatment for chronic primary pain, specifically because it works on the nervous system rather than just the tissues.
- A whole-person approach that addresses the nervous system, not just the site of pain, tends to be more effective for long-term relief.
What Is Pain? Understanding the Body's Alarm System
Think of pain as your body's alarm system.
When you're injured, nerves send signals through your spinal cord to your brain. Your brain interprets those signals and creates the sensation of pain. This system exists to protect you, and most of the time, it does its job well.
The confusion starts when that alarm keeps firing after the danger has passed.
Pain science has shown us that chronic pain isn't simply about damaged tissue. It's often about how the nervous system is processing signals, and sometimes, the system itself becomes the problem rather than the thing it was designed to detect.
NICE guidance: The National Institute for Health and Care Excellence categorises chronic pain into two main types. Secondary pain is caused by an underlying condition such as arthritis or endometriosis. Chronic primary pain is where the pain itself is the main condition: think fibromyalgia, or chronic neck and back pain with no clear structural cause. NICE specifically recommends acupuncture for chronic primary pain (NG193, 2021), because it targets nervous system regulation rather than tissue repair alone.
The Purpose of Pain in Healing
Acute pain plays an important role in recovery.
If you sprain an ankle or touch something hot, pain tells you to stop, protect the area, and allow healing to begin. It's usually sharp, linked to a specific event, and as healing progresses, it settles.
When that process doesn't happen as expected, it's often a sign that something else is going on. Not that you've done anything wrong. Not that you're not trying hard enough. The system that's meant to quiet down simply hasn't had the chance to do so yet.
Acute vs. Chronic Pain: The Key Differences
The main difference between acute and chronic pain is duration and purpose. The infographic below summarises this clearly, followed by a more detailed breakdown.

Understanding the difference between acute and chronic pain
| Feature | Acute Pain | Chronic Pain |
|---|
| Duration | Short-term (less than 3 months) | Long-term (more than 3 months) |
| Purpose | Warning signal of injury or illness | No longer serves a protective purpose |
| Cause | Usually linked to a specific event | Can follow injury, illness, or have no obvious cause |
| Resolution | Goes away as the body heals | Persists after healing is complete |
| Impact | Temporary disruption | Can affect mood, sleep, and daily life long-term |
| Focus of care | Tissue healing | Nervous system regulation and quality of life |
In the clinic, I commonly see people trying to manage chronic pain as though it were still acute: resting more, waiting for it to pass, pushing through on good days and crashing on bad ones. That approach makes sense for a short-term injury. For chronic pain, it often isn't enough.
When Does Pain Become Chronic? Understanding the Timeline
Pain rarely becomes chronic overnight. It's usually a gradual shift: signals that don't quiet down when expected, a body that seems to have forgotten how to feel safe again.
Clinically, the three-month threshold exists because most tissues heal within that window. If pain remains intense or unpredictable after that time, it's likely that the nervous system is still responding as if danger is present, even when the original injury has healed.
That doesn't mean the pain isn't real. It means the alarm hasn't fully stood down yet.
At this point, support usually shifts from waiting for pain to resolve to actively helping the nervous system calm and regulate. That is a meaningful distinction, and understanding it can take some of the self-blame out of the experience.
Why Some Pain Doesn't Go Away After Healing
This is one of the most common questions I hear from clients across Teesside, and one of the most distressing to sit with.
Many people feel confused, or quietly dismissed, when scans come back normal and yet the pain continues. I want to be clear about something: normal scan results do not mean the pain isn't real. They often mean the problem has shifted from the site of injury to the nervous system itself.
This is known as central sensitisation. The brain and spinal cord stay on high alert. Pain pathways become more responsive. Non-painful stimuli may start to feel uncomfortable. Smaller triggers cause bigger responses.
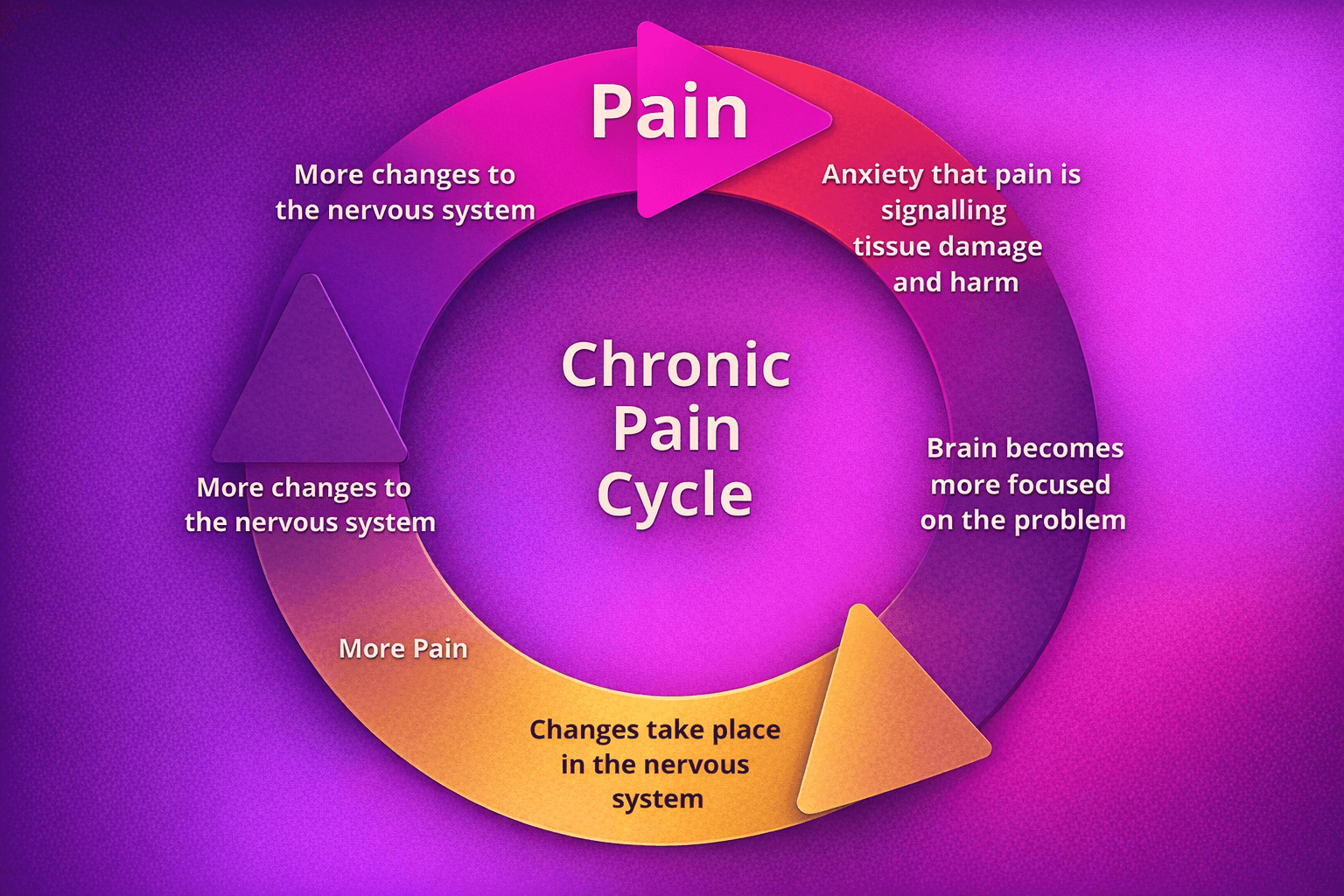
The chronic pain cycle: how nervous system sensitisation keeps pain going
In practice, central sensitisation can look like this:
- Pain that spreads beyond the original site of injury
- Sensitivity to touch, temperature, or pressure that seems out of proportion
- Feeling "wired" or easily overwhelmed alongside the physical pain
- Pain that fluctuates unpredictably, regardless of activity level
Understanding central sensitisation often brings genuine relief to people: not because it fixes anything immediately, but because it explains why pain can persist without visible damage. It's a real, physical change in how the nervous system is functioning. And it can be worked with.
Recognising the Signs That Pain Has Become Chronic
People with persistent pain often notice more than just the pain itself. Common accompanying signs include:
- Poor or broken sleep
- Ongoing fatigue that rest doesn't resolve
- Irritability or low mood
- Gradual reduction in movement and activity
- Difficulty concentrating
If pain has lasted more than twelve weeks and these symptoms are present, that's a conversation worth having: with your GP, and potentially with a practitioner experienced in chronic pain support.
I also notice subtler signs earlier in the process. Pain that lingers a little longer than expected. A growing focus on discomfort between sessions. Avoiding movement not because it hurts to move, but because of fear of what might happen if you do. That pattern, where life starts to shrink around the pain, is often a signal that early support could interrupt the cycle before it becomes more entrenched.
What Causes Chronic Pain? Exploring the Underlying Factors
Chronic pain rarely has a single cause. It can develop after injury, illness, inflammation, or prolonged stress. Sometimes there isn't a clear starting point at all.
What matters most is understanding what's maintaining the pain now, not just what triggered it originally.
The Role of Injuries, Illness, and Inflammation
Long-term inflammatory conditions such as arthritis or endometriosis can drive ongoing pain directly. Past injuries that didn't fully settle can also leave lasting sensitivity in the nervous system.
In the clinic in Middlesbrough, I regularly work with people whose musculoskeletal pain started with a clear injury, such as a fall, a car accident, or a sports injury, that stayed long after the tissues had healed. Sometimes even short-term illnesses can leave behind nerve sensitivity that takes longer to resolve than anyone expected.
How Stress and Emotional Load Contribute
The connection between emotional state and pain experience is powerful, and it's not just psychological: it is physiological.
High levels of stress activate the body's threat response. That same response also amplifies pain signals. The nervous system doesn't distinguish clearly between physical danger and emotional distress: both turn up the volume.
Living with constant pain is also emotionally exhausting. The pain leads to frustration, isolation, and disrupted sleep. Those states, in turn, make the nervous system more sensitive. It becomes a cycle that's difficult to break without addressing both sides.
This is something I see regularly in clinic. People arrive managing the physical pain, through ice packs, painkillers, and careful movement, but the emotional load is carrying just as much weight. Addressing that isn't a soft option. It's part of what makes treatment effective.
The Mind-Body Connection and Pain Persistence
Your thoughts, beliefs, and emotions have a direct impact on physical sensation, and chronic pain is one of the clearest examples of this.
If you've spent months or years in pain, your brain becomes increasingly focused on threat signals. That hypervigilance is not a character flaw. It's an adaptation. The nervous system has learned, correctly, that pain is a regular feature of your life, and it is trying to protect you by staying alert to it.
Therapies like cognitive behavioural therapy (CBT) and mindfulness don't treat pain by dismissing it. They work by changing your relationship to it, shifting the nervous system out of that constant threat response and creating more space between stimulus and reaction.
In our acupuncture work for chronic pain in Middlesbrough, this is a dimension we always consider. Treatment that only addresses the physical site of pain, while leaving the nervous system on high alert, tends to have a ceiling. Working with the whole system, including the emotional and stress load, is where more lasting change tends to happen.
Pulse diagnosis: reading the body's deeper patterns
The Traditional Chinese Medicine Perspective on Chronic Pain
Western medicine primarily views chronic pain through the lens of the nervous system and structural issues. Traditional Chinese Medicine offers a different, complementary framework, one that has been used to understand persistent pain for thousands of years.
In TCM, pain is often understood through the phrase: "Bu tong ze tong, tong ze bu tong" which translates as: "If there is no free flow, there is pain; if there is free flow, there is no pain."
This core principle suggests that pain arises when the flow of Qi and blood becomes stagnant or blocked. That stagnation can be caused by injury, emotional stress, cold, or environmental factors. The qualities of the pain, whether sharp, dull, fixed, or moving, provide diagnostic information about the nature of the imbalance and where to focus treatment.
Acupuncture works to stimulate specific points on the body to restore the smooth flow of Qi and blood, regulate the nervous system, and improve circulation. Rather than focusing solely on the site of pain, TCM considers how that pain is interacting with the whole system.
Integrating TCM and Western Approaches
You don't have to choose between Western healthcare and Traditional Chinese Medicine. Many people find that the most effective approach brings both together.
One distinction worth making clearly: not all needlework is the same. In the clinic, I often meet people who've said they've "tried acupuncture" when what they actually had was dry needling as part of a physiotherapy session. Dry needling is a useful tool for targeting tight muscles and trigger points. Traditional Chinese Acupuncture is a complete medical system with a different framework and treatment intention, one that considers how your nervous system, circulation, emotional state, and overall pattern are all contributing to your experience of pain.
"This integrative approach gives you more angles to work from, and in my clinical experience, more sustainable results."
Frequently Asked Questions
How long does pain need to last before it's considered chronic?
Pain is generally considered chronic when it lasts or recurs for more than three months. This timeframe is used because most tissues heal within that window. After three months, if pain continues, it is likely that the nervous system, rather than active tissue damage, is now the main driver, and that calls for a different approach to treatment.
Why does pain sometimes continue when scans show nothing wrong?
This is very common, and it's one of the most confusing aspects of chronic pain. When scans come back clear, it doesn't mean the pain isn't real. It often means the problem has shifted to the central nervous system itself, a process called central sensitisation, where pain pathways have become more responsive and continue firing without new injury. Understanding this is usually a turning point for people.
Can acupuncture help with chronic pain?
Yes. NICE recommends acupuncture as a first-line treatment for chronic primary pain, specifically because it works on the nervous system rather than just the tissues. A 2018 meta-analysis by Vickers et al. in the Journal of Pain, drawing on over 20,000 patients across 39 randomised controlled trials, found acupuncture significantly outperformed both sham treatment and standard care for musculoskeletal pain, osteoarthritis, and chronic headache, with effects that persisted at one-year follow-up. At our chronic pain acupuncture clinic in Middlesbrough, we offer both Traditional Chinese Acupuncture with Deanna and Battlefield Acupuncture with Anthony, depending on what's most appropriate for your situation.
How does stress make chronic pain worse?
Stress activates the body's threat response, the same system that amplifies pain signals. A nervous system under sustained emotional or psychological load stays on high alert, which lowers the pain threshold and can make existing pain feel more intense. This isn't a mental health problem separate from the pain: it's a physiological interaction. Addressing stress and emotional load is part of effective chronic pain support, not an optional extra.
What's the difference between fibromyalgia and other types of chronic pain?
Fibromyalgia is classified as a chronic primary pain condition, meaning the pain itself is the main issue rather than a symptom of identifiable tissue damage or an underlying disease. It's characterised by widespread muscular pain, fatigue, and heightened sensitivity, all consistent with central sensitisation. It responds well to approaches that target nervous system regulation, which is why acupuncture is increasingly used alongside other management strategies for fibromyalgia.
★★★★★
"I'd had lower back pain for three years and tried everything. Physio helped temporarily but it always came back. After six sessions with Deanna I genuinely woke up one morning and realised the pain had gone. I couldn't quite believe it."
Google Review · Verified Patient · Middlesbrough
Final Thoughts
Chronic pain can be deeply disruptive: physically, emotionally, and in ways that are hard to explain to people who haven't experienced it.
Understanding when pain becomes chronic matters not to give it a label, but to shift the focus from "why isn't this better yet?" to "what does my system need now?" Those are very different questions, and the second one tends to lead somewhere more useful.
Persistent pain often reflects nervous system changes rather than ongoing tissue damage. That's important, because it means the right kind of support, the kind that works with your whole system rather than just the site of pain, can make a meaningful difference, even when pain has been present for a long time.
Written byDeanna Thomas
MBAcC · CNHC Registered · PSA Accredited · PG Diploma Obstetrics & Gynaecology · Fertility Support Trained
Deanna is a licensed acupuncturist and the founder of Deanna Thomas – Acupuncture & Wellbeing, based at The House in Middlesbrough. She specialises in fertility, women's health, and chronic pain, and is trained in reproductive immunology through the Fertility Support programme led by Naava Carman. Her practice is grounded in Traditional Chinese Medicine and informed by current clinical evidence.
Ready to Try a Different Approach?
If chronic pain has become a fixture in your life, it may need a different kind of care than a short-term injury. Find out more about our whole-person approach to acupuncture for chronic pain in Middlesbrough, including what to expect, which practitioner might be the right fit, and how we approach treatment at The House.
See Chronic Pain Acupuncture "Wellness grows where energy flows."